© 2024 Embrace Hospice and Home Health
All Rights Reserved
All Rights Reserved
In today’s day and age, it’s highly likely that you, a loved one, a family member, a friend, a neighbor or a coworker are dealing with chronic pain – and you’re by no means alone. It’s estimated that over 50 million Americans are affected by chronic pain, and over 20 million are affected by high-impact chronic pain, meaning it interferes with their life and work on a daily basis. As pain becomes increasingly widespread to the point that many individuals treat chronic aches and pains as the norm, it must be addressed.
September is Pain Awareness Month, a month dedicated to raising awareness about the prevalence of pain and pain management. Given that the prevalence of pain increases with age, a particularly important community of individuals who require proper pain management is individuals under hospice care, or end of life care.

As individuals and their families make the decision to embrace hospice care, the concern of pain and discomfort that often accompanies end-stage disease is among the top. Hospice care is a service that is centered around providing your loved one, family member or friend maximal comfort as they near the end of their life. Pain management is a key component of hospice care, ensuring that individuals are free from pain, which provides them with not only physical, but also mental, relief.
Despite the great potential and aid that hospice provides, a recent study revealed that upwards of 60% of individuals in hospice care still deal with pain, and that one third of the individuals from a collection of studies rated their pain as moderate or severe. Unresolved pain means that somewhere in the system, there are interferences with proper pain management measures. These barriers may come from the family and patient, or they may come from the healthcare providers, or a combination of both in some cases. Several things that may impede pain management from the side of the family includes denial of pain as a means of protection from acknowledging end of life, acceptance that pain is just part of the disease and can’t be resolved, fear of addiction, cognitive restrictions, or feeling a need to be “brave”. From the healthcare providers’ side, barriers include poor pain assessments, not recognizing the global nature of pain, fear of addiction, fear of legal issues, or fear of doing harm to name a few. Any number of these barriers can result in mismanaged pain and discomfort in the patient. Managing and controlling pain lends an impactful hand in making sure your loved one’s end of life remains high quality. It is imperative that you are aware of these barriers to pain relief, so that they can be addressed and reduced.
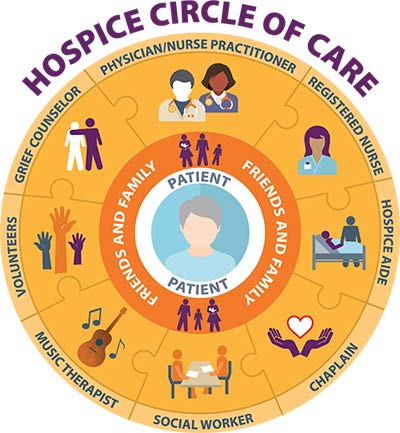
Pain management in hospice comes in many forms. Hospice care is provided by a multidisciplinary team of healthcare professionals, to include doctors, nurses, pharmacists, spiritual counselors, social workers, bereavement specialists, and other special support. Together, these professionals can collaborate and devise an individualized pain plan to facilitate comfort within an individual’s own home. While doctors and pharmacists can provide medications to alleviate physical pain, other key members of the hospice team can address other areas in an individual’s life that inspire comfort on a deeper level. Pain goes beyond just the physical mechanism, and individuals experiencing high levels of pain can often benefit from an all-encompassing approach to relief. This includes providing spiritual support and a professional who can assist in acceptance and grief. Taking a multidimensional approach to pain management is an incredibly effective way of reducing pain while increasing quality of life.
When discussing physical pain, there are several important factors to remember. Everyone’s pain threshold is different and cannot be judged by an outsider. All pain deserves to be treated and relieved. Consider using a 1-10 scale to understand your loved one’s pain – with 1 being no pain at all and 10 being the worst pain they have ever experienced. Pain should be treated immediately, as delaying treatment only makes the pain worse. Finally, while a fear of addiction is common when it comes to pain management, it is not likely to occur when medications are used properly under the supervision of healthcare providers.
Understanding the benefit that pain management has on an individual’s quality of life towards the end and the prevalence of pain in older individuals in America, it is crucial to stay vigilant against the barriers that may interfere with pain management. Be sure to get involved with your loved one’s hospice care and include yourself in the planning process. You and your loved one are a vital part of the interdisciplinary team.
Sources:
Image 1 – https://anest.ufl.edu/2020/09/08/september-is-pain-awareness-month/
Image 2 – https://www.ecommunity.com/services/post-acute-care/community-hospice
International Association for the Study of Pain – https://www.iasp-pain.org/advocacy/pain-awareness-month/
American Society for Pain Management http://www.aspmn.org/Documents/Position%20Statements/Pain%20Management%20at%20the%20End%20of%20Life%202017.pdf
Johns Hopkins Medicine – https://www.hopkinsmedicine.org/health/wellness-and-prevention/palliative-care-methods-for-controlling-pain